
Peritoneal dialysis

- Medically reviewed by
- AKF's Medical Advisory Committee
- Last updated
- March 4, 2026
Jump to
How does peritoneal dialysis (PD) work?
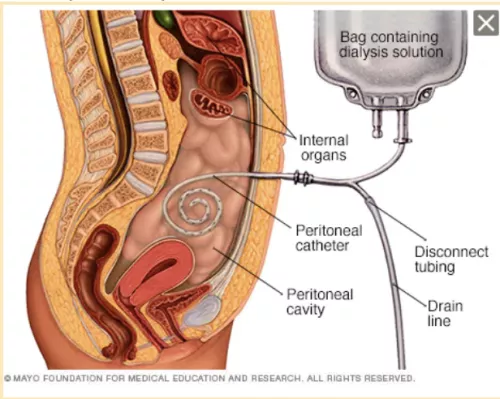
- During PD, you use a catheter to fill your belly with a cleaning fluid called dialysate. A catheter is a thin tube that transports fluid in or out of your body. The tissue that covers most of the organs in your belly (the peritoneum) acts as a filter for this process.
- The dialysate will stay in your belly for a period of time, usually four to six hours, while it cleans your blood. This time is called a dwell time.
- Then, you will drain the used dialysate out of your belly and refill it with fresh dialysate. This process is called an exchange. You may do these exchanges yourself or with the help of a machine. Your doctor will tell you how many exchanges you should do each day.
In PD, you will always have dialysate in your belly, unless you are doing an exchange. During your dwell time, you are free to move around and do your daily activities while the dialysate sits in your belly.
What is dialysate?
Dialysate is a liquid with sugar in it that pulls fluid and waste from your blood. The dialysate holds on to the waste and fluid and removes them from your body when you do an exchange.
How does the catheter get into my belly?
Before you start PD, doctors will do a small surgery to put the catheter into your belly. The end of the catheter will come out through your skin, either on your belly or your chest. Usually, you can stay awake during this surgery — doctors will numb the area of your body where they put in the catheter so you do not feel any pain.
What are the types of PD?
The two most common types of PD are continuous cycler-assisted peritoneal dialysis (CCPD) and continuous ambulatory peritoneal dialysis (CAPD).
Use this table to help you compare the two types of PD:
| Continuous cycler-assisted PD (CCPD) | Continuous ambulatory PD (CAPD) |
How does it work? | CCPD uses a machine called a cycler to do your exchanges. | CAPD uses gravity to help you do the exchanges by hand. |
When do I need to do it? | CCPD is usually done at night, while you sleep. You have to do it every night. | CAPD is done during the day because you need to do each exchange yourself. You have to do it every day. |
How often do I need to do exchanges? | Usually, the cycler does three to five exchanges each night. In the morning, the machine will fill your belly with dialysate to let it sit in your belly during the day, until you go to bed and start your nightly CCPD treatment again. Your doctor will tell you:
A dialysis nurse or technician can show you how to set up the cycler to give you the right treatment.
| Most people do four exchanges each day. Between exchanges, the dialysate will sit in your belly for the dwell time. At the end of the day, you will fill your belly one last time and let the dialysate sit in your belly while you sleep. In the morning, you will start exchanges again. Your doctor will tell you:
|
How long do exchanges take? | It takes about nine hours for the cycler to complete three to five exchanges. | It takes about 30–40 minutes to drain and refill your belly with dialysate for each of the four exchanges. |
Where can I do it? | You will likely do CCPD in your bedroom while you sleep. | You can choose any room in your home, workplace or other space that is clean and dry. |
How can I do PD safely?
Doing PD has many benefits, such as going about your daily activities between exchanges and not having to travel to a center for dialysis. To stay healthy and safe while doing PD, keep the following tips in mind.
Care for your catheter to prevent infection
An infection in your belly (called peritonitis) is the most common problem that may happen when doing PD. Infections can happen when bacteria get into your belly around your catheter. Bacteria may also get into your catheter while you connect or disconnect it from your dialysate bags.
To help prevent infection:
- Wash your hands well with soap and warm water before touching your catheter.
- Clean the area where your catheter goes into your body with antibiotic cleanser every day. Ask your doctor or nurse which cleanser to use.
- Keep your catheter dry. Most doctors recommend you avoid swimming, but you can take showers once the skin has fully healed after the catheter surgery.
- Wear a surgical mask over your nose and mouth while you do exchanges.
- Only do exchanges in clean, dry places.
Your doctor or nurse will teach you how to best care for your catheter.
If you notice any signs of infection, call your doctor right away to get treatment. Signs of infection include:
- Fever
- Chills
- Belly pain
- Redness, pain or swelling in the area around your catheter
- Dialysate that looks cloudy or off-color when you drain it from your belly
Do PD in a clean, dry space
Choose a space for doing your exchanges that:
- Is clean and dry
- Is well lit
- Has a clean table or shelf for your supplies
- Is free of plants, which can grow mold or bacteria that can raise your chance of infections
Keep pets out of the room
For most of us, pets are family. You do not have to find a new home for your pets because you are starting PD. However, you should keep pets out of the room you choose for doing exchanges to make sure it stays as clean as possible.
Read this blog post to learn more about pets and peritoneal dialysis.
Create a safe storage space for your supplies
Store your PD supplies in a clean, dry space that is easy for you to get to. Make sure children and pets cannot get to your supplies.
Supplies are usually delivered to your home once a month. Each delivery might include many large, heavy boxes. If you cannot lift heavy boxes, make sure you have someone to help you on delivery day.
How long can I stay on PD?
How long you can stay on PD depends on many things, such as your overall health and how well you follow your treatment plan. Many people live on dialysis for years. If your health gets worse while you are on PD, you may have to switch to hemodialysis or get a kidney transplant.
Can I continue my usual activities?

Probably. PD can offer a lot of flexibility. If you do PD at night, you will have more time for other activities during the day, but there are some limits on what you can do. To keep your catheter area dry and prevent infection, you should avoid swimming or using hot tubs. If those are activities you enjoy, talk to your doctor about a treatment plan that might let you continue those activities.
Working while doing PD
To prepare for doing PD at work, talk to your employer to:
- Set up a clean and dry space where you can do exchanges.
- Work out a schedule so you can follow your treatment plan.
Your health and well-being depend on you doing all the exchanges recommended by your doctor. If needed, your social worker may be able to help you work out an agreement with your employer.
Traveling while doing PD
One of the benefits of doing PD is being able to travel without having to look for a dialysis center at your destination. Usually, your PD supplies can be shipped to the place where you are staying. Learn more about traveling considerations for people with kidney disease.
Is PD or hemodialysis right for me?
Hemodialysis is another type of dialysis in which a machine is used to filter waste and extra fluids from your blood.
There are many things to consider when deciding which kind of dialysis is right for you, such as:
- Your overall health
- Your work schedule
- Activities you enjoy
- Your living situation — some people may prefer to do dialysis at home, while some may find it easier to go to a dialysis center for treatments
Talk to your doctor to help you make a treatment plan that works for your life.

